Frequently Asked Questions - FAQ
|

|
1 General information
2 Measurement Methods
3 Physiology
4 Application
1 General information
1.1 What is O2C (oxygen to see)? |
 |
The O2C (oxygen to see) was developed by LEA Medizintechnik. It is a combination of a laser Doppler flowmeter and a tissue spectrometer. With this device it is possible to measure simultaneously in different measurement depths blood flow, blood flow velocity, oxygen saturation and relative amount of haemoglobin in the measurement tissue. The O2C version O2C-OF is the succession of the OptoFlow. The O2C version O2C-ATS is the succession of the AbTisSpec.
1.2 What is the OptoFlow? |
 |
The device named OptoFlow was developed by LEA Medizintechnik. It contains a laser doppler flowmeter which measures simultaneously in different measurement depths with only one probe. The OptoFlow has been integrated into the O2C (oxygen to see) in the year 2002.
1.3 What is the AbTisSpec? |
 |
The name AbTisSpec is an acronym for absorption tissue spectrophotometer. This device was developed by LEA Medizintechnik. It is an advancement of the EMPHO in the measurement of the microvascular oxygen saturation of haemoglobin in the tissue. Additionally the AbTisSpec measures the relative amount of haemoglobin in the tissue. The spectrophotometry of the AbTisSpec has been increased from the detection of visible light to the detection of near infrared radiation. This technology was integrated to the O2C(oxygen to see) in the year 2002.
1.4 What is the EMPHO? |
 |
The name EMPHO is an acronym for the Erlanger microlightguide photometer. This device was developed by the Institute of physiology and cardiology Erlangen in the late 80's. The EMPHO is a tissue spectrometer which is illuminating the tissue and calculates the microvascular oxygen saturation of haemoglobin by detection of the backscattered light. In the 90's the EMPHO has been produced and distributed by the company Diehl (Nürnberg) and following by the company Bodensee-Gerätewerk (Überlingen). In the late 90's the production has been given up.
1.5 How does it compare to other methods? |
 |
| Method |
Parameter |
Disadvantage |
| O2C oxygen to see |
determines oxygen saturation, amount of haemoglobin and blood flow at the venous part of the capillaries. Information about the metabolism of tissue |
local Microcirculation |
|
| Blood gas analysis: SvO2 |
determines mixed venous oxygen saturation of the whole body or of one organ, depending on the vein. Does not determine local oxygen saturation in tissue. |
global |
Heterogeneity of organ perfusion and influence of shunt blood. |
| Pulseoximetry |
determines arterial oxygen saturation, and is a measure for saturation of blood with oxygen in the lung, therefore the lung function. |
global |
No information about local hypoxia (as venous saturation is not determined) and locally delivered amount of oxygen (as perfusion not determined). |
|
Ultrasound Doppler |
determines blood flow in big vessels. |
local Macrocirculation |
local heterogeneity in supplied organ, microangiopathies; is only indirect indicator for hypoxia. |
| Angiography |
determines anatomy of supply vessels. |
local Macrocirculation |
hemodynamic relevance of stenosis, local heterogeneity of organ; is only indirect indicator for hypoxia. |
| Plethysmography |
determines blood flow in whole extremities |
local Macrocirculation |
|
| Nail fold microscopy |
makes capillaries visible and their pathologic changes. With additional video systems blood flow velocity can be determined. |
local Microcirculation |
expensive, cannot be used everywhere in the body, only determines flow in single capillaries. |
| pO2 tissue oxygen partial pressure |
determines pO2 transcutaneously or with needle probes subcutaneously. Gives the mixed value of arterial, venous and tissue-pO2. |
local Microcirculation |
transcutane electrode influences measurement by heating, needle probe by tissue trauma. Both are influenced easily by arterial pO2, so that hypoxia in critical venous areas ("lethal corner") can be overseen. Reason for pO2 change (delivery or consumption) cannot be determined. |
| NIR-Spectrometry |
determines optically oxygen saturation, especially in capillary-venous area of microcirculation similar to the spectrometric method that is used by the O2C. |
local Microcirculation |
Reason for SO2 change (delivery or consumption) cannot be determined. |
| Laser Doppler |
determines blood flow in the microcirculation either punctual or by a scanner over a certain tissue area. |
local Microcirculation |
low penetration depth, instability. Indirect indicator for hypoxia. |
1.6 Is it reproducible? |
 |
Several studies concerning reproducibility, evaluation and validation had been conducted for the O2C (oxygen to see).
Among others the correlation with Microspheres and cerebral venous oxygen saturation had been shown. Blood flow velocity, as well as local oxygen saturation measured with O2C correlated well with perfusion measurement by microspheres and cerebral venous oxygen saturation.
Reproducibility Studies had shown no significant changes during this observation period.
2 Measurement Methods
2.1 Why does O2C not show 100% oxygen saturation? What is the difference to the pulse oximeter? |
 |
O2C measures in the capillary-venous part of the vascular tree. These are the vessels that carry the blood back from the organ to the heart after distribution of oxygen and nutrients to the cells. Therefore they carry the oxygen which was not consumed by the cells. This oxygen reflects the "oxygen reserve". In the whole body it is about 75%. Still in the microcirculation it can be much lower, because of local heterogeneities. Undersupply ("hypoxia") occurs first in the capillary-venous areas ("lethal corner"), therefore O2C is very sensitive to tissue hypoxia.
Pulse oximetry determines arterial oxygen saturation, that means the amount of oxygen that is in the vessels leading to the organs. Arteries transport oxygen from the lung (through the heart) to the tissue, before distribution of the oxygen to the cells. Therefore arterial oxygen saturation is a measure for oxygen saturation of blood in the lung, and therefore lung function. Arterial oxygen saturation is about 98-100% in a person with healthy lungs. With pulse oximeter local oxygen undersupply cannot be determined, as hypoxia occurs after distribution of oxygen to the organs in areas with the lowest oxygen saturation, the capillary-venous area.
The difference between arterial and venous oxygen saturation ("arterial-venous difference"), that means the oxygen extraction, amounts to 25% in the whole body. This applies for the macrocirculation, if blood is drawn from aorta and caval vein. The venous blood includes "shunt-blood" (blood that has not passed oxygen consuming cells, but is directly flowing from arteries into veins) and blood of organs with completely different oxygen extraction (high heterogeneity of organs). Therefore it does not allow determination of oxygen extraction of certain organs.
To determine extraction of single organs it would be necessary to draw blood from the artery and vein of the organ of interest. The difference would be the local oxygen extraction. Still it is often not feasible to draw blood of single organs. Also in the organ there are also heterogeneities that are not reflected by oxygen measurements in single vessels. With O2C, however, it is possible to determine capillary-venous oxygen saturation and therefore extraction, if arterial oxygen saturation is known. Now it is possible to determine changes in local oxygen extraction and together with blood flow oxygen consumption.
For determination of changes of local oxygen consumption (metabolism), it is necessary to measure both, local oxygen saturation and local blood flow.
2.2 What is the difference to the pO2 Electrode? |
 |
The pO2 is a common measure for dissolved oxygen in tissue. It depends on constant parameters like solubility coefficient of blood and cells, and also on the amount of oxygen that is released by haemoglobin, the oxygen carrier in blood. Under normal conditions almost all oxygen is carried by haemoglobin to the tissue and the capacity of blood to carry oxygen physically dissolved is very low. In the tissue the oxygen is released by the haemoglobin, physically dissolved and diffuses into tissue. If haemoglobin is highly saturated with oxygen a small drop in oxygen saturation causes a big drop in pO2 according the "oxygen binding curve". Therefore changes in pO2 do not reflect actual changes in oxygen saturation and amount of released oxygen. The amount of oxygen that is transported into tissue therefore is only characterised by changes in oxygen saturation.
Oxygen saturation usually drops in a linear way along the organ supplying vessels (as each unit of tissue consumes the same amount of oxygen), whereas pO2 drops exponentially (due to the hyperbolic oxygen binding curve).
pO2 electrodes determine a mixed value of arterial, venous and tissue pO2. Because of the exponential drop, the influence of the arterial part of the vessel system is higher than changes in tissue or capillary pO2. Hypoxic areas can be overseen.
As pO2-electrodes determine present amount of oxygen, they do not distinguish between oxygen supply and consumption.
Transcutaneous pO2 electrodes influence measurement results also by heating of measurement area. Heating causes vasodilatation and increasement of blood flow. Therefore oxygen extraction decreases and values shift to more arterial oxygen saturation. Subcutaneous pO2 electrodes influence measurements by insertion into tissue and cause tissue trauma.
2.3 What is the difference between tissue spectroscopy with two wavelengths and oxygen measurement of O2C with several hundreds of wavelengths? |
 |
A similar method like oxygen saturation measurements with O2C is near-infrared spectroscopy as used by NIRO of Hamamatsu. An important difference to the O2C is the measured and processed wavelength range.
For that you have to know something about influence of tissue on light passing through tissue. On its way through tissue light is absorbed by different tissue chromophores and partly scattered by mitochondria. As well absorption as scattering changes the amount of light of certain wavelengths, that is returning from tissue to the detector and can be measured. Absorption, that is mainly caused by blood, causes certain changes in spectra of the whole measured wavelength range, as well as scattering and other tissue chromophores cause specific changes.
Certain wavelengths are more influenced by one or another factor. If you are only looking at a few wavelengths it is difficult to determine which factor caused the change in intensity of measured light and different properties of light have to be used for calculation (e.g. phase differences of light). But if you observe the whole wavelength range, you can quantify the influence of different factors by analysis of shape changes of the spectra. O2C determines all wavelength of visible range that are changed by blood. Therefore changes in scattering properties of the tissue, that influence spectra at specific wave lengths, can be determined in each measurement and taken into account in each calculation.
2.4 What is measurement depth of O2C? |
 |
This questions can only be answered at the moment by mathematical calculations and measurements at models. Light moves in tissue more easily in the forward direction than in the backward direction. That means that light that is immitted into tissue e.g. a finger rather can be seen at the other side of the finger coming out, than at the side where the light has been immitted. This makes measurements in "remission" - back to the surface - more difficult than in "transmission" through tissue. Light that is backscattered to the surface moved - much simplified - in a semicircular path through tissue. Therefore measurement depth mainly depends on the distance of immitting to detecting lightguide. In near-infrared wavelength range mathematical models showed, that a glass fibre separation of 400-800 µm collects light of blood of the upper dermis (1). With a separation of 2,5 cm a measurement depth of 2 cm in brain could be achieved (2). In a model with Intralipid (2%) and haemoglobin (0.28 g/dl) a measurement depth of 3.4 mm with a separation of 6 mm could be shown (3).
Measurement depth depends on optical properties of tissue, of amount of blood and probe geometry. The exact measurement depth therefore cannot be determined, but it is clear, that measurements with two different separations allow two different measurement depths (deep and superficial), as possible with the O2C probes. That is the way it should be described. Physiological reactions (e.g. perfusion increase during work) indicate, that with current design muscle perfusion can be determined with deep measurement depths.
The difference to laser Doppler scanning has to be emphasised: laser Doppler scanning is a method that produces maps of perfusion. As here light is not directly coupled into tissue, mainly the part of the light is measured, that is reflected at the surface of skin and has a penetration depth of few micrometers. Measurement volume is accordingly small and unrepresentative, a problem that can only in part be compensated by scanning technique.
- 1 Meglinksky IV, Matcher SJ. Modelling the sampling volume for skin blood oxygenation measurements
Med Biol Eng Comput, 39(1):44-50, 2001
- 2 Luo Q, Nioka S, Chance B. Functional Near-Infra Red Imager
SPIE 2979: 84- 93, 1997
- 3 Dissertation, Alfons Krug, Quantitative optische Gewebemessungen am Herzen und an der Leber
Friedrich-Alexander-Universität Erlangen-Nürnberg, p. 73-84. 1998
2.5 How fast is O2C? |
 |
Update of measurement values in monitoring window each two seconds.
Update in beat-to-beat window each 50 ms.
For comparison: Conventional pO2-Electrode: about 20 minutes equilibration time.
3 Physiology
3.1 How does O2C measure capillary-venous and what information does that provide? |
 |
Information of the capillary venous area of the vessels, meaning the vessels that transport blood after distribution of oxygen to the organs/cells, is gathered with the O2C. The reason is, that light is absorbed by vessels bigger than about 100 µm and does not return to the detector system (1). Therefore only the smallest vessel of nutritive organ supply (microcirculation) is measured (arterioles, capillaries, venoles). As about 85% of the blood is in the capillary-venous system (2), O2C measurements represent mainly this area. Therefore oxygen supply is determined locally in the organ and not globally.
- 1 Gandjbakhche, A.H., Bonner, R. F., Arai, A. E., Balaban, R. S., Visible-light photon migration through myocardium in vivo
Am. J. Physiol. 277 (46): H698-H704, 1999
- 2 Burton A.C., The vascular bed. In: Physiology and biophysics of the circulation
Chicago, IL: Year Book Medical, 1965
3.2 Why is it important to measure simultaneously oxygen saturation and blood flow? |
 |
The measured oxygen saturation is the percentage amount of oxygen bound on haemoglobin.
This is important for the diagnosis of tissue hypoxia, as the physically dissolved oxygen can be measured directly by a measurement of oxygen saturation. This is made possible by the oxygen binding curve of the haemoglobin.
If you want to know, how much oxygen is absolutely available, you additionally need the blood flow. With this information it is possible to determine oxygen uptake by tissue, when absolute amount of inflow (by blood flow and arterial oxygen saturation) and absolute amount of outflow (by blood flow and capillary venous oxygen saturation) can be determined.
Reasons for decreased oxygen saturation, that are increased oxygen uptake or decreased blood flow, can be determined.
If you measure blood flow only, you can determine the amount of delivered oxygen. But there is no information gained about availability of oxygen in the capillary venous system.
4 Application
4.1 Can the probe be used intracorporally? |
 |
The probes can be used in the gastrointestinal tract with an endoscope, a feeding tube, a plastic protective sleeve or without any aid.
4.2 What is important for application of the probe? |
 |
Blood flow measurements are influenced by movement. Application without any movement is necessary for valid measurements. SO2 and Hb measurements are independent of movement and therefore stable even under difficult conditions.
Frequent mistakes during blood flow measurements are:
- Movement at the probe tubing due to insufficient strain relief
- Movement artefacts by respiration movements, if the hand or arm is lying on thorax or touching it (particularly difficult during measurements in the gut or moving organs)
- Not visible muscle shivering of the patient.
Oxygen saturation measurements are influenced by colours and light:
- Frequent mistakes: coloured disinfectant (there is also uncoloured disinfectant in the OR, if you insist on it), especially directly after surgery at intensive care units (wash of the colour before measurement).
- Influence of external light: Cover probe with blanket, if direct surgery light shines on measurement point. Always control hemoglobin spectra (correct spectra see manual)!!
All measurements of microcirculation are influenced by pressure:
- Frequent mistake: Application of the probe with too much pressure on tissue. Radial application of tape can cause venous congestion!
4.3 What do my measurements mean? |
 |
Provocation, therapy or disease leads to:
| Symptom |
Blood flow |
Haemoglobin amount |
Oxygen saturation |
Cause |
| 1. Slow decrease of blood flow |
Slow decrease of blood flow |
Increase of haemoglobin amount |
Slow decrease of SO2 |
-> Venous congestion |
| 2. Decrease of blood flow and SO2 |
Decrease of blood flow |
Small decrease or no change of haemoglobin amount |
Decrease of SO2 |
-> Arterial ischemia |
| 3. Measurement in a tumour: |
High blood flow |
High haemoglobin amount |
Low SO2 |
-> high metabolism |
| 4. Measurement in an open wound: |
High blood flow |
High haemoglobin amount |
High SO2 |
-> hyperaemia as sign of inflammation |
| 5. A diabetic patient shows following parameter at the leg: |
High blood flow |
Normal (or high) haemoglobin amount |
High SO2 |
-> Hyperaemia caused by vegetative neuropathy |
| 6. An arteriosclerotic patient shows following parameter at the leg: |
Low blood flow |
Low haemoglobin amount |
Low SO2 |
-> arterial ischemia |
| 7. An arteriosclerotic patient shows following parameter at the leg: |
Low blood flow |
Low haemoglobin amount |
Very high SO2 |
-> Tissue with low metabolism caused by ischemic damage |
| 8. An arteriosclerotic patient shows following parameter at the leg: |
no stable values and a spectrum as shown here:
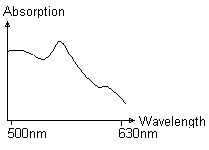 |
The spectrum is no haemoglobin spectrum, but a cytochrome spectrum of reduced cytochromes, i.e. the tissue is no longer supplied by oxygen.
The calculated values are invalid! |
4.4 What are normal values? |
 |
Measurement values depend on skin temperature and emotional activation of the patient.
Following tables are showing reference values:
Finger/Toe:
| |
Normal values |
Critical values |
| rHb |
35-90 AU |
<15 AU oder >90 AU |
| SO2 |
70-90% |
<10% |
| Blood Flow |
10-200 |
<5 AU |
Arm/Leg:
| |
Normal values |
Critical values |
| rHb |
35-90 AU |
<15 AU oder >90 AU |
| SO2 |
20-50% |
<10% |
| Blood Flow |
10-50 |
<5 AU |
Perfusion at different skin sites in comparison:
Finger(warm) > Face > Arm > Leg
4.5 What does AU mean? |
 |
The abbreviation A.U. used for the units of blood flow and blood flow velocity means "Arbitrary Units". These are units that are chosen arbitrarily by the developer of the device.
The reason for the introduction of "Arbitrary Units" is based on the origin of the values.
The measured signals for blood flow are electrical values of frequencies and amplitudes, so that the unit would be a combination of electrical units. Therefore usually a new unit for blood flow is introduced. To calculate the blood flow in ml/min, it would be necessary to compare the electrical signals with a method that measures the blood flow in ml/min (e.g. plethysmography, microspheres) for each organ (or organs with similar optical properties). Then the arbitrary units can be converted in ml/min. This "calibration" has to be done at the measured organ, as there is no artificial model at the moment, that simulates tissue in a realistic way.
The same applies for the unit of haemoglobin rHb [A.U.].
4.6 Does ambient light affect the readings? |
 |
No, normally the probe darkens an area big enough, so ambient light does not affect the readings. The O2C (oxygen to see) displays the haemoglobin spectra online at the screen. So you can always check whether you got an adverse effect by ambient light.
The laser-Doppler measurements of the O2C (oxygen to see) has an ambient light compensation algorithm. Nevertheless the measurement can be influenced by ambient light.
4.7 What resolution does the measurement have? |
 |
Oxygen saturation
Measurement range 0- 100 % absolute measurement
Resolution +/- 1 %
Amount of haemoglobin
Measurement range 0 - 120 AU (arbitrary unit) relative measurement
Resolution +/- 1 AU
blood flow velocity
Measurement range 0 - 4000 AU (arbitrary unit) relative measurement
Resolution +/- 1 AU






















